As the COVID-19 pandemic continues to wreak havoc across the world, some of you may be wondering what happens to single-use medical equipment once it’s been used.
This article explores the topic of medical waste in the UK, outlines the various types, and explains what happens to each at the end of its lifetime.
In particular, with regards to the coronavirus outbreak, there is currently a lot of discussion around PPE, which stands for Personal Protective Equipment. This will be covered below.
Medical waste must be dealt with separately from general waste. This is to avoid the spread of infection and to prevent the general public and the environment from coming to any harm as a result of the waste.
What is medical waste?
There are four categories of medical waste in the UK:
- Infectious
- Sharps
- Anatomical
- Medicine (redundant)
Each waste type must be stored in separate containers and is then regularly collected by waste management companies and dealt with in the manner required by law.
Infectious waste
Infectious waste is the most common medical waste type created by hospitals and PPE falls into this category.
PPE is any personal equipment which aids health and safety in the workplace and so for doctors and nurses on the frontline, PPE means items such as gloves, aprons, gowns, facemasks, respirators, and eye protection.
Alongside PPE, infectious waste can include anything contaminated with blood, pus, saliva, mucous, faeces, urine, vomit, skin, or tissue.
Any waste related to COVID-19 immediately falls into this category.
Infectious waste is placed in dedicated thick plastic bags which are then sealed and placed in large plastic bins. These bins are kept locked and collected by a medical waste management company.
Hard infectious waste is sent for incineration and softer infectious waste is either sent for incineration too or steam sterilisation in an autoclave.
Sharps waste
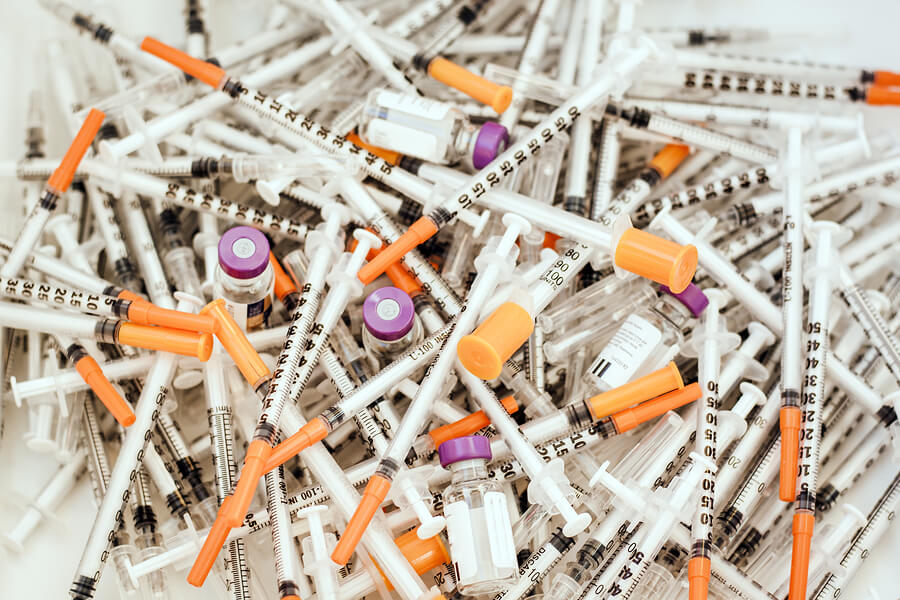
Sharps waste is a biomedical waste category that includes any object used to puncture or lacerate the skin — or with the potential to do so. This can include, but isn’t limited to:
- Hypodermic needles
- Shards of bone or teeth
- Staples
- Pins
- Clamps
- Metal wire
- Scissors
- Disposable scalpels and blades
- Knives
Sharps waste is high risk as it could easily puncture the skin of anyone handling it and so it is stored in plastic containers.
Aside from physical harm, sharp waste could also lead to infection due to the purpose of the items involved — traces of blood, for example, could be present on items such as hypodermic needles.
Alongside hospitals and GP surgeries, sharps waste is often collected from nursing homes, tattoo and piercing premises, schools, the beauty and cosmetic industry, the food industry, and the clothing industry.
In medical settings, sharps waste is often placed directly into a yellow plastic sharps container, clearly marked with the British safety number 7320 and UN 3291.
Sharps containers are removed from use when three-quarters full and the container is then sealed before collection takes place.
Sharps waste is often incinerated in case of infection, or some medical centres separate the sharps into infectious and non-infectious waste — only incinerating the infectious sharps.
Anatomical waste
Anatomical waste is unique to the healthcare field and includes human or animal body parts, organs, and blood — including heavily soaked dressings.
Body parts are stored in secure refrigerated units and the rest of the waste is collected in plastic bags which are then placed inside plastic containers — often locked wheelie bins.
Anatomical waste is sent for incineration at a suitably authorised facility. It is transported there inside special UN-approved containers.
Medicine waste

This final waste category is redundant medicine and is separated into a further two categories: hazardous and non-hazardous.
The hazardous medicine contains cytotoxic and cytostatic drugs; non-hazardous medicine doesn’t.
Medicine containing cytotoxic and cytostatic drugs is often collected in a yellow plastic sharps container, clearly labelled.
Each medical centre deals with redundant medicine in a different manner.
